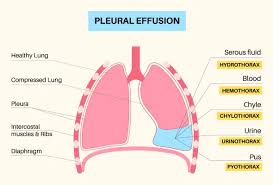
Pleural Effusion is the abnormal accumulation of fluid within the pleural cavity, the space between the lungs and chest wall. Normally, only a small amount of lubricating fluid is present, but when balance between fluid production and absorption is disturbed, effusion develops. It can result from various causes such as heart failure, pneumonia, malignancy, tuberculosis, liver cirrhosis, or pulmonary embolism.
There are two main types: transudative effusion, caused by systemic factors like increased hydrostatic pressure or decreased oncotic pressure, and exudative effusion, resulting from local inflammation, infection, or malignancy. Common symptoms include shortness of breath, chest pain (often sharp and worsened by breathing), cough, and reduced exercise tolerance. On examination, decreased breath sounds, dullness to percussion, and reduced chest expansion are typical findings.
Diagnosis is confirmed through chest X-ray, ultrasound, or CT scan, followed by thoracentesis, where fluid is aspirated and analyzed to determine its nature. Treatment depends on the underlying cause: diuretics for heart failure, antibiotics for infection, or drainage procedures for large or malignant effusions. In some cases, pleurodesis or indwelling pleural catheters are required. Prompt recognition and management are essential to relieve symptoms and prevent complications.