INTRODUCTION
Locomotor ataxia may sound like a complex medical term, but its impact is deeply human and palpable…it’s the silent thief of steady steps and graceful movement. Imagine trying to walk while your body can’t quite tell where its limbs are without looking. For those with locomotor ataxia, this is a daily reality marked by unsteady and uncoordinated walking that challenges independence and balance.
WHAT IS LOCOMOTOR ATAXIA?
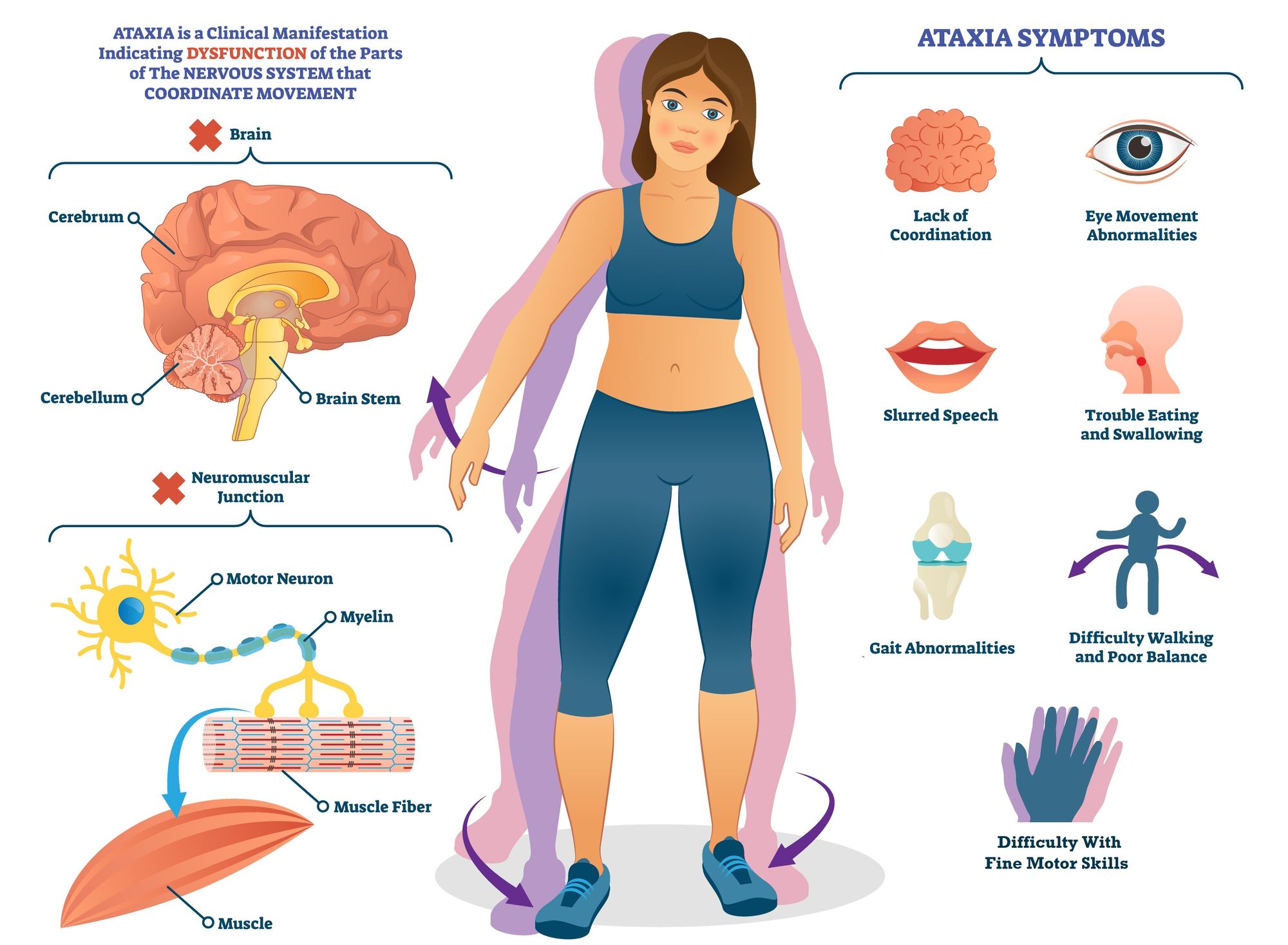
Locomotor ataxia is a neurological condition characterized by loss of coordination primarily due to impaired sensory pathways that carry information about the position of the body in space—called proprioception. When these pathways are damaged, the brain lacks the feedback needed to coordinate muscle movements properly, resulting in an unsteady, staggering gait often described as wide-based and irregular. Unlike cerebellar ataxia, which comes from cerebellum dysfunction, locomotor ataxia is mainly due to damage in the posterior roots and spinal cord.
CAUSES OF LOCOMOTOR ATAXIA
Historically, locomotor ataxia was most famously linked to tabes dorsalis, a late manifestation of untreated syphilis caused by the bacterium Treponema pallidum. This infection damages the dorsal spinal roots, impairing proprioception and causing the classic symptoms of locomotor ataxia. Today, other causes include:
- Nutritional deficiencies such as vitamin B12 or vitamin E deficiency
- Chemotherapy drugs like vincristine or cisplatin that damage nerves
- Autoimmune or paraneoplastic conditions attacking sensory nerves
- Peripheral neuropathies due to diabetes or other systemic diseases
- Less common causes include trauma, infections, or tumors affecting sensory pathways.
RECOGNIZING SYMPTOMS
The hallmark symptom is an unsteady gait, often described as “stomping” or “lurching” steps. Patients tend to look down at their feet to compensate for the loss of proprioception, often worsening in the dark or on uneven surfaces. Additional symptoms can include:
- Limb numbness and “lightning” shooting pains
- Positive Romberg’s sign (instability when standing with feet together and eyes closed)
- Difficulty with fine motor tasks due to impaired limb sensation
- Sensory loss in limbs, decreased reflexes
- Visual dependence and impaired balance leading to frequent falls.
HOW IS IT DIAGNOSED?
Diagnosis involves a thorough medical history, physical and neurological examination focusing on coordination, reflexes, muscle strength, and sensory testing. Confirmatory tests may include:
- MRI or CT scans to identify central nervous system pathology
- Blood tests to detect infections, vitamin deficiencies, or autoimmune markers
- Lumbar puncture for cerebrospinal fluid assessment in cases of infection
- Electrophysiological studies to assess nerve function
- Genetic testing if hereditary ataxias are suspected .
TREATMENT AND MANAGEMENT
Though locomotor ataxia can progress, early recognition and management improve quality of life. Treatment includes:
- Addressing underlying causes, like antibiotics for neurosyphilis or vitamin supplementation
- Physical therapy focusing on muscle coordination retraining using techniques such as Frenkel exercises, which teach patients to consciously control movements through repetition and visual feedback
- Assistive devices like walkers or canes to enhance stability
- Multidisciplinary care involving occupational therapy and speech therapy for associated difficulties.
LIVING WITH LOCOMOTOR ATAXIA: HOPE AND ADAPTATION
Living with locomotor ataxia demands resilience. Though challenging, improvements through rehab and adaptive strategies empower patients to maintain independence. Understanding the condition better can help caregivers and providers support navigation of this complex neurological landscape.Locomotor ataxia, a condition that disrupts the simple act of walking, reminds us how intricate and vital our sensory systems are. With advances in diagnosis, therapy, and supportive care, those affected can find pathways toward improved balance and movement, transforming an invisible struggle into a journey of hope.