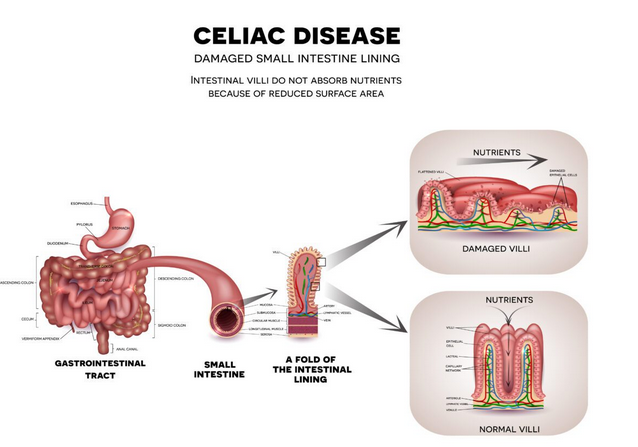
🌾 Celiac Disease: Causes, Symptoms, Risks, and Recovery:
Celiac disease is a serious autoimmune disorder that affects millions of people worldwide. It is triggered by consuming gluten, a protein found in wheat, barley, and rye. For individuals with celiac disease, eating gluten causes the immune system to attack the small intestine, leading to damage, nutrient malabsorption, and a wide range of health problems.
This blog will explore why and how celiac disease happens, who’s at risk, what diseases it can lead to, and how to manage it naturally and medically.
❓ Why Celiac Disease Happens
Celiac disease occurs when the body’s immune system overreacts to gluten. It is believed to be caused by a combination of genetic predisposition and environmental triggers. Individuals with specific genetic markers (mainly HLA-DQ2 or HLA-DQ8 genes) are more likely to develop the disease.
However, not everyone with these genes will develop celiac, indicating that other factors like infections, gut health, or gut permeability (“leaky gut”) may also play a role.
🔍 How Celiac Disease Happens
When someone with celiac disease eats gluten, the immune system mistakenly attacks the villi — small finger-like projections in the small intestine that absorb nutrients. This immune response leads to:
-
Inflammation in the small intestine
-
Damage to intestinal lining
-
Nutrient deficiencies
-
Systemic symptoms beyond the gut
This is not the same as a gluten intolerance or wheat allergy — celiac is an autoimmune condition and can have long-term complications if left unmanaged.
⚠️ Diseases and Complications Caused by Celiac Disease
If untreated, celiac disease can lead to serious health issues:
-
Malnutrition (due to poor nutrient absorption)
-
Iron-deficiency anemia
-
Osteoporosis or osteopenia (from calcium and vitamin D loss)
-
Infertility and miscarriage
-
Liver disease
-
Lactose intolerance
-
Neurological disorders (e.g., peripheral neuropathy, ataxia)
-
Skin conditions (e.g., dermatitis herpetiformis)
-
Increased risk of intestinal cancers
👶 Age and Health Conditions at Risk
Celiac disease can occur at any age, from infancy to adulthood, and some people are more at risk:
High-Risk Groups:
-
People with a family history of celiac disease
-
Individuals with other autoimmune diseases (e.g., Type 1 diabetes, autoimmune thyroid disease, Addison’s disease)
-
Those with Down syndrome, Turner syndrome, or Williams syndrome
-
People with micronutrient deficiencies of unknown cause
-
Infants introduced to gluten early or with early gut infections
💊 Medical Sources for Recovery and Management
There is no cure for celiac disease, but it can be effectively managed by eliminating gluten completely from the diet.
1. Strict Gluten-Free Diet
This is the only proven treatment. It requires lifetime avoidance of all foods containing wheat, barley, rye, and contaminated oats.
2. Nutritional Support
-
Supplements for deficiencies (e.g., iron, calcium, B12, vitamin D)
-
Regular blood tests to monitor healing and nutrient levels
3. Doctor & Dietitian Support
-
Consult a gastroenterologist for diagnosis and follow-up
-
Work with a registered dietitian to build a balanced, gluten-free meal plan
🌿 Natural Sources for Supportive Recovery
Once gluten is removed from the diet, the body begins to heal naturally. These natural supports can accelerate healing and ease symptoms:
Gut-Healing Foods:
-
Bone broth – Rich in collagen and amino acids
-
Fermented foods (yogurt, kefir, sauerkraut) – Promote gut bacteria
-
Leafy greens – High in fiber and nutrients
-
Sweet potatoes, carrots – Soothing, nutrient-dense
-
Bananas, applesauce, rice – Gentle on inflamed gut
Natural Supplements:
-
L-glutamine – Helps repair the intestinal lining
-
Probiotics – Support microbiome health
-
Omega-3s – Reduce inflammation
⚠️ Always consult a doctor before adding supplements, especially in autoimmune conditions.
🛡️ Tips to Prevent Celiac Disease
You can’t prevent celiac disease if you are genetically predisposed, but you can delay onset or reduce severity by:
-
Breastfeeding while introducing gluten to infants (may lower risk)
-
Avoiding unnecessary antibiotics or NSAIDs that disrupt gut health
-
Supporting gut health through diet and probiotics
-
Managing stress, which can weaken immune balance
-
Seeking early diagnosis in family members if symptoms appear
🚨 Common Symptoms of Celiac Disease
Celiac symptoms vary widely and can affect many parts of the body.
Digestive Symptoms:
-
Bloating and gas
-
Diarrhea or constipation
-
Abdominal pain
-
Nausea or vomiting
Non-Digestive Symptoms:
-
Fatigue
-
Weight loss
-
Anemia
-
Depression or anxiety
-
Brain fog or difficulty concentrating
-
Skin rash (dermatitis herpetiformis)
-
Delayed growth in children
-
Irregular menstrual cycles or infertility
Many adults with celiac may have no gut symptoms, making it harder to detect.
🧪 How Is Celiac Disease Diagnosed?
Diagnosis typically includes:
-
Blood Tests
-
tTG-IgA (tissue transglutaminase antibodies)
-
EMA-IgA (endomysial antibodies)
-
-
Endoscopy with Biopsy
-
To confirm damage to the small intestine
-
Important: Do not stop eating gluten before testing, as this may result in false negatives.
🧠 Emotional and Mental Health in Celiac Disease
Living with celiac disease means being constantly vigilant. It can cause:
-
Social anxiety (eating out, traveling)
-
Depression from lifestyle changes
-
Food guilt or fear
Tips for emotional support:
-
Join local or online support groups
-
Learn to cook gluten-free meals
-
Empower yourself with knowledge
-
Celebrate healing milestones
✅ Quick Recap: What to Do If You Suspect Celiac Disease
-
✅ Talk to your doctor before removing gluten
-
✅ Get tested through blood tests and biopsy
-
✅ If diagnosed, follow a strict gluten-free diet
-
✅ Monitor nutrient levels and gut healing
-
✅ Seek support from professionals and peers