Introduction:
Infantile convulsions, also known as seizures in infants, can be one of the most frightening experiences for parents and caregivers. A convulsion happens when the brain cells send sudden, abnormal electrical signals, causing the baby’s body to stiffen, jerk, or become unresponsive for a short time. While many seizures in infants are harmless and temporary (such as febrile seizures due to fever), others may point to underlying medical issues that need attention.
This blog aims to help parents understand the causes, symptoms, management, and care of infantile convulsions in simple words.
What Are Infantile Convulsions?
An infantile convulsion is a seizure episode that occurs in a child under 1 year of age. It is not a disease itself but a symptom of something affecting the brain.
There are two broad types:
Febrile Convulsions – Triggered by fever, usually harmless and common in children 6 months to 5 years.
Epileptic Seizures – Due to abnormal brain activity, may require long-term treatment.
Common Causes:
- Genetic Disorders: Conditions such as Tuberous Sclerosis Complex or other gene mutations can lead to infantile convulsions.
- Brain Malformations: Abnormalities in how the brain develops, whether before or after birth, can be a trigger.
- Brain Injury: This can include injury from a lack of oxygen (hypoxic-ischemic encephalopathy) during delivery or from other significant brain trauma.
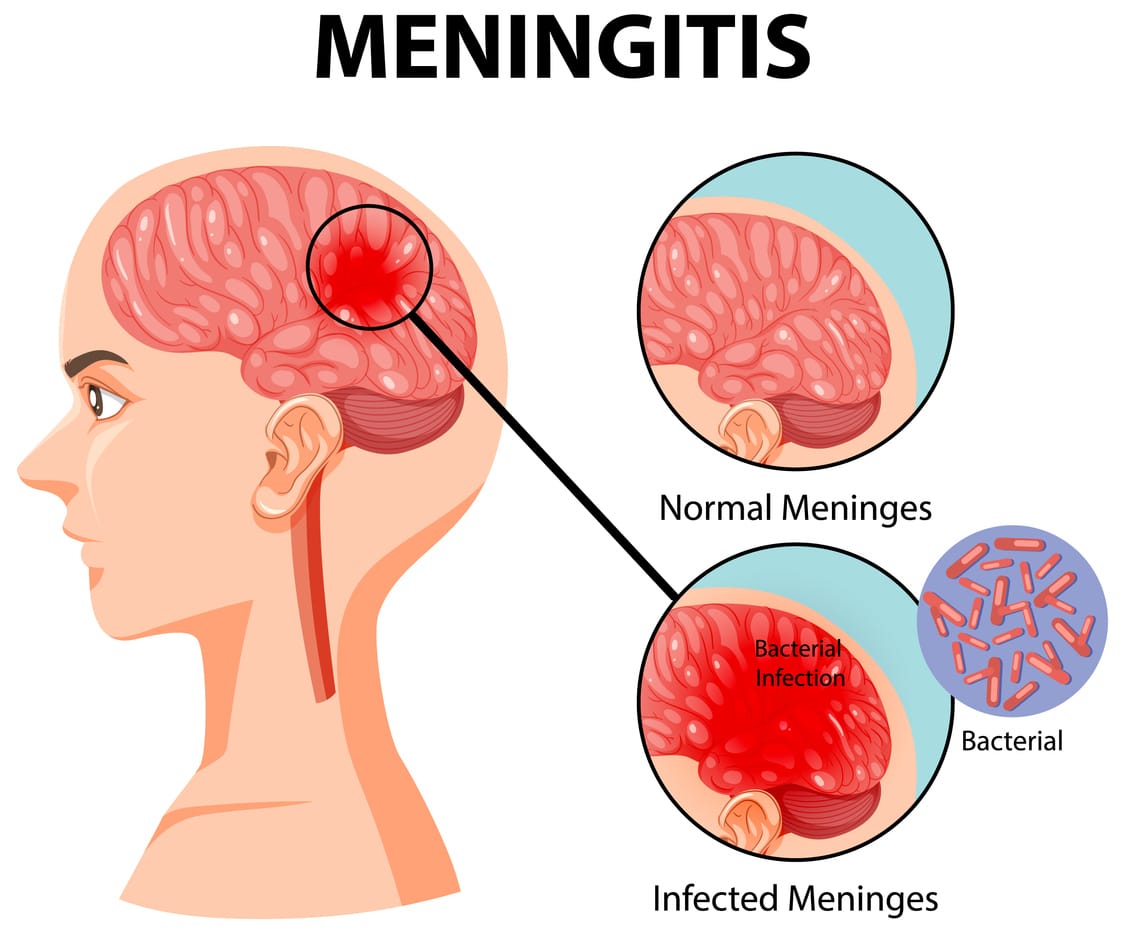
- Infections: Brain infections like meningitis or encephalitis can cause infantile spasms.
- Metabolic Disorders: These are disorders affecting the body’s metabolism that can affect brain function.
- Abnormal Blood Vessels: Problems with the brain’s blood vessels, such as an arteriovenous malformation, can be a cause.
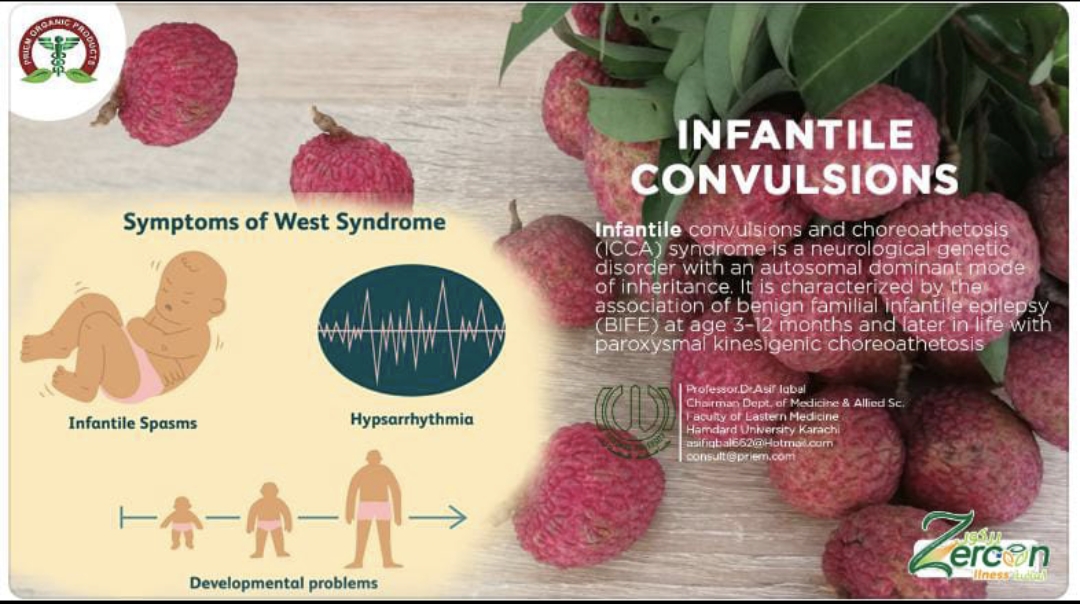
Common Signs and Symptoms
Sudden Body Movements: Brief, sudden jerks or a stiffening of the baby’s muscles.
Head Nodding: A quick, repeated nodding of the head.
Limb and Trunk Jerks: Arms and legs may bend, extend, or be thrown outward.
Back Arching: The infant may arch their back during a spasm.
Eye Changes: Eyes may roll upward, or a baby might develop wide-eyed blinks.
Clustering: Spasms often occur in clusters, with many spasms happening one after another.
Timing: Symptoms are most common right after a baby wakes up or while falling asleep.
Developmental Issues: Parents may notice a temporary loss of previously acquired skills, such as smiling or sitting up.
Diagnosis
- Doctors usually perform the following to find the cause:
- Medical history (family history, recent fever, trauma).
- Blood tests (to check glucose, calcium, electrolytes).
- EEG (Electroencephalogram) – To study brain activity.
- MRI or CT scan – To rule out structural problems.
When to See a Doctor
Recognizing infantile spasms can be challenging because they are often subtle and can be mistaken for normal reflexes or common conditions like acid reflux. If you notice sudden, brief jerking movements in your infant, especially in clusters, contact their doctor immediately. A prompt diagnosis is crucial, and a doctor can perform a neurological exam and anelectroencephalogram (EEG) to confirm infantile spasms.
Management & First Aid During a Convulsion
The most important step is to stay calm and protect the baby.
- ✔️ Place the baby on a flat, safe surface.
- ✔️ Turn the baby gently on their side to prevent choking.
- ✔️ Loosen tight clothing.
- ✔️ Remove nearby objects to avoid injury.
- ✔️ Note the duration of the seizure.
- ✔️ Call emergency services if the seizure lasts more than 5 minutes.
❌ Do NOT put anything in the baby’s mouth.
❌ Do NOT shake or try to hold the baby still.
Diet for Infants with Convulsions
While medication is the main treatment for seizures, nutrition can support brain health and reduce risk factors. Parents should consult a pediatrician or nutritionist before making dietary changes, but here are some general guidelines:
- Breastfeeding → Best for the first 6 months.
- Iron-rich foods → Lentils, spinach, fortified cereals, pureed meats.
- Calcium & magnesium → Yogurt, cheese, bananas, oats.
- Brain boosters → Omega-3 rich fish (salmon, well-cooked, boneless), nuts & seeds paste.
- Fruits & veggies → Bananas, apples, carrots, pumpkin, peas (soft/mashed).
- Special diet → Ketogenic diet only under doctor’s supervision in epilepsy cases.
- Avoid → Processed/junk foods, excess sugar, caffeine, and preservatives.
Conclusion
Infantile convulsions can be alarming, but not all seizures mean lifelong illness. Many children, especially those with febrile seizures, outgrow them with time. The key is early recognition, calm management, and seeking medical advice.
As parents and caregivers, knowing how to act during a seizure can make a life-saving difference. Stay informed, stay calm, and never hesitate to consult a healthcare professional.