Chronic Obstructive Pulmonary Disease (COPD) & Nutrition: The Overlooked Link in Respiratory Health
Breathing is something most of us take for granted — until it becomes difficult. Chronic Obstructive Pulmonary Disease (COPD) is one such condition that silently limits millions of lives worldwide. More than just a lung disease, COPD is a progressive condition influenced by lifestyle, environment, and nutrition.
According to the World Health Organization (WHO), COPD is the third leading cause of death globally, responsible for approximately 3.2 million deaths in 2019. Despite its prevalence, COPD remains underdiagnosed and undertreated, especially in low- and middle-income countries. In Pakistan, COPD is a growing health concern. High rates of tobacco smoking, indoor air pollution from biomass fuel (wood, coal, dung cakes), and worsening urban air quality contribute significantly to the burden. Limited awareness and delayed diagnosis further challenge effective management.
This blog explores the causes, symptoms, management strategies, and the often-overlooked role of nutrition in improving outcomes for COPD patients
Chronic Obstructive Pulmonary Disease:
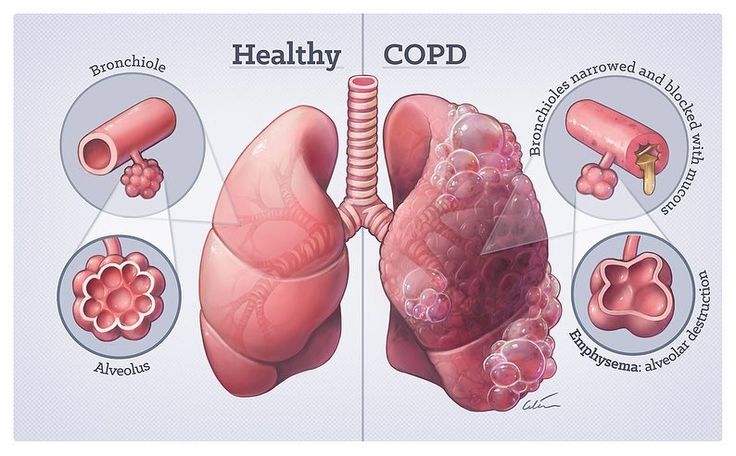
Chronic Obstructive Pulmonary Disease (COPD) is a long-term lung disease that makes it hard to breathe because airflow in and out of the lungs is partly blocked.
It mainly includes two conditions:
• Chronic bronchitis → swelling and narrowing of the airways with excess mucus.
• Emphysema → damage to the air sacs (alveoli) in the lungs, reducing oxygen exchange.
Etiology and Risk Factors:
· Tobacco smoking – the single greatest risk factor.
· Occupational exposures – dust, chemicals, fumes.
· Environmental pollution – particularly in urban populations.
· Genetic predisposition – e.g., alpha-1 antitrypsin deficiency.
· Childhood respiratory infections – impairing lung development.
Clinical Manifestations:
· Persistent dyspnea (shortness of breath).
· Chronic productive cough.
· Wheezing, chest tightness, and reduced exercise tolerance.
· Frequent exacerbations leading to hospitalization.
Diagnosis:
· Spirometry (key tool): post-bronchodilator FEV1/FVC ratio < 0.70.
· Supportive assessments: chest imaging, arterial blood gases, and comorbidity evaluation.
Management Strategies:
1. Smoking cessation – most effective intervention.
2. Pharmacological therapy – bronchodilators, anticholinergics, corticosteroids (as indicated).
3. Pulmonary rehabilitation – exercise, education, breathing strategies.
4. Vaccination – influenza and pneumococcal.
5. Oxygen therapy – for patients with hypoxemia.
6. Surgical options – in advanced, refractory cases.
👉 While medications and rehabilitation are central to COPD care, an equally important but often overlooked component is nutrition.
Why Nutrition Matters in COPD?
Nutrition directly influences breathing, immunity, and energy balance in COPD patients. Malnutrition leads to muscle wasting (including respiratory muscles), while obesity makes breathing more difficult. Both conditions worsen patient outcomes.
A well-balanced diet:
· Preserves lung and muscle strength.
· Improves exercise tolerance.
· Reduces frequency of exacerbations.
· Enhances overall quality of life.
Nutritional Interventions in COPD:
1. Energy Balance:
· Increased breathing effort raises calorie needs.
· Aim to maintain a healthy BMI (21–25) with individualized calorie intake.
2. Macronutrient Focus:
· Protein: 1.2–1.5 g/kg/day for muscle preservation.
· Carbohydrates: choose complex sources (avoid excess → ↑ CO₂ production).
· Fats: MUFA/PUFA provide energy without raising CO₂ load.
3. Micronutrients & Antioxidants:
· Vitamin D, calcium, magnesium → support bones and muscles.
· Antioxidant-rich foods (fruits, vegetables, nuts, seeds) → reduce inflammation and oxidative stress.
4. Practical Feeding Strategies:
· Small, frequent meals reduce pressure on the lungs.
· Avoid gas-forming foods (carbonated drinks, beans, fried snacks).
· Maintain adequate hydration unless restricted.
5. Specialized Support:
· Malnourished patients may require oral nutrition supplements (ONS).
· Referral to a dietitian ensures individualized plans.
Sample Diet Plan for COPD Patients:
Breakfast:
1 boiled egg or 2 egg whites (protein for muscle strength)
1 slice whole wheat bread or chapati
A small bowl of seasonal fruit (e.g., papaya, apple, pear)
Green tea or herbal tea (avoid too much caffeine)
Mid-Morning Snack:
Handful of soaked almonds or walnuts
Fresh fruit juice (without added sugar) OR lassi (light, not heavy)
Lunch:
1–2 small chapatis or ½ cup brown rice
Grilled/baked chicken, fish, or lentils (protein source)
Cooked vegetables (carrot, pumpkin, spinach, bottle gourd)
Salad (cucumber, tomato, carrot)
Evening Snack:
Yogurt with chia seeds
OR vegetable soup (light, warm, easy to digest)
Dinner:
1 chapati or small bowl of rice
Moong daal / chicken curry (less oil, less spice)
Steamed vegetables
A small bowl of salad
Before Bed:
Warm milk with a pinch of turmeric
OR a few soaked dates if energy is low
Nutrition Tips for COPD:
· Eat small, frequent meals (large meals can make breathing harder).
· Focus on high-protein foods (chicken, fish, eggs, daal, beans).
· Stay hydrated to keep mucus thin.
· Avoid fried, oily, spicy foods (they increase breathlessness and reflux).
· Limit salt to reduce water retention and swelling.
· If underweight → add high-calorie healthy snacks (nuts, milkshakes).
· If overweight → control portions to reduce lung stress.
Public Health and Professional Relevance:
COPD poses a significant economic and social burden due to frequent hospitalizations, reduced productivity, and high healthcare costs.
· Early detection with spirometry screening is crucial.
· Patient education empowers lifestyle change.
· Nutritional therapy improves exercise tolerance, reduces exacerbations, and enhances quality of life.
· In Pakistan, strengthening tobacco control, improving indoor air quality, and increasing awareness about nutrition can make a measurable difference.
Conclusion:
COPD is preventable and manageable with a comprehensive, multidisciplinary approach. Alongside medications, rehabilitation, and lifestyle modification, nutrition is a cornerstone of care. By maintaining muscle strength, reducing exacerbations, and improving quality of life, nutritional strategies help patients breathe easier and live healthier lives.
Healthcare professionals must prioritize early diagnosis, holistic management, and nutrition-focused care to combat the growing burden of COPD, especially in countries like Pakistan.