- Office Hour : 09:00am - 6:00pm
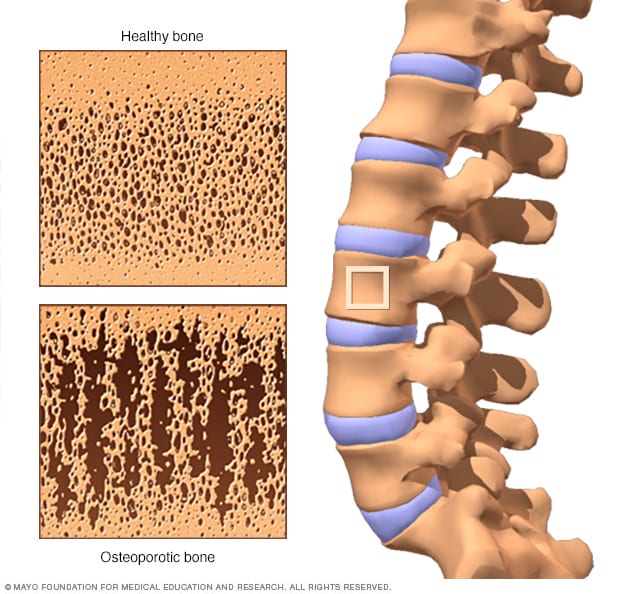
OSTEOPOROSIS
Osteoporosis is a condition where bones become weak and fragile, increasing the risk of fractures. It often develops silently and is most common in older adults, especially women. Nutrition plays a key role in both prevention and management of this disease.
Calcium and vitamin D are the two most important nutrients for strong bones. Dairy products, leafy green vegetables, almonds, and fortified foods are excellent sources of calcium. Vitamin D, obtained from sunlight, fish, and eggs, helps the body absorb calcium effectively.
Protein, magnesium, and vitamin K also support bone strength, while excess caffeine, soft drinks, and high salt intake can weaken bones. Maintaining a healthy weight, staying active with weight-bearing exercises, and eating balanced meals are essential strategies.
Good nutrition not only slows bone loss but also reduces fracture risk. A diet rich in bone-friendly nutrients truly builds a stronger foundation for lifelong health.
What is cancer? by nutritionist Mehak Zahir
What Is Cancer?
Cancer is one of the most feared words in the world. Cancer is not just one disease — it’s a group of over 100 different diseases that all involve uncontrolled growth of abnormal cells in the body.
Normally, your body’s cells grow, divide, and die in a very organized way. Old or damaged cells are removed, and new ones take their place.
But in cancer, this process breaks down. Cells:
- Start growing out of control
- Don’t die when they should
- May invade nearby tissues
- Can even spread (metastasize) to other parts of the body
This uncontrolled growth forms tumors (except in cancers like leukemia, which affect blood and bone marrow).
What Causes Cancer?
Cancer is caused by changes (called mutations) in the DNA inside your cells. DNA is like your cell’s instruction manual — and when it gets damaged, the cell may start acting abnormally.
These mutations can be:
- Inherited (from your parents)
- Acquired during life (due to environment, lifestyle, or random error)
Common Risk Factors:
| Risk Factor | How it contributes |
| Smoking | Linked to lung, mouth, throat, and many other cancers |
| Obesity | Creates chronic inflammation and hormonal imbalances |
| Poor Diet | Lack of fiber, antioxidants; excess sugar or processed meat |
| Alcohol | Increases risk for liver, breast, and esophageal cancer |
| Radiation | UV rays (skin cancer), X-rays, and environmental exposure |
| Infections | HPV (cervical cancer), Hepatitis B/C (liver cancer), H. pylori (stomach) |
These factors don’t guarantee cancer will develop — but they significantly increase risk.
How Does Cancer Grow?
Cancer begins with one damaged cell that ignores the body’s normal rules. Here’s a simplified step-by-step:
- DNA Mutation happens in a single cell.
- That cell begins to divide uncontrollably.
- A tumor forms as the abnormal cells pile up.
- The tumor may grow its own blood vessels to feed itself (angiogenesis).
- It can invade nearby tissues and eventually spread through blood or lymph.
Chronic diseases by Nutritionist Maryam Noman
CHRONIC DISEASES:
Chronic diseases, also called non-communicable diseases (NCDs), are long-term health conditions that usually progress slowly and last for years, often for a lifetime. Unlike infections that can be cured with short-term treatment, chronic diseases often require ongoing management and lifestyle adjustments.
Common Examples of Chronic Diseases
Cardiovascular diseases (heart attack, stroke, hypertension)
Diabetes
Cancer
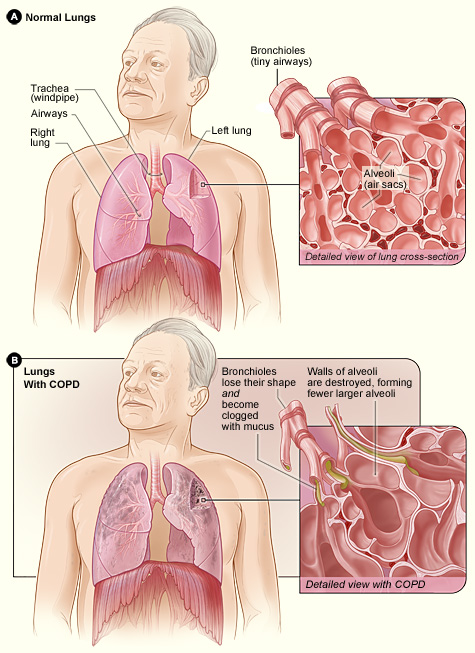
Chronic respiratory diseases (asthma, COPD)
Arthritis and osteoporosis
Chronic kidney disease
Causes and Risk Factors
While genetics can play a role, many chronic diseases are linked to lifestyle and environmental factors such as:
Unhealthy diet (high sugar, salt, and processed foods)
Physical inactivity
Tobacco use
Excessive alcohol consumption
Stress and poor sleep habits
Environmental pollution
Impact on Individuals and Society
Chronic diseases not only affect a person’s health but also have emotional, social, and financial impacts. They reduce quality of life, limit productivity, and lead to high medical costs. Globally, chronic diseases are the leading cause of death and disability.
Prevention and Management
The good news is that most chronic diseases are preventable or manageable through:
Healthy eating – focus on fruits, vegetables, whole grains, and lean proteins.
Regular physical activity – at least 30 minutes a day.
Avoiding smoking and excessive alcohol use.
Routine health checkups for early detection.
Stress management through meditation, yoga, or hobbies.
The Role of Awareness
Raising awareness about chronic diseases is key to reducing their burden. Public health programs, community support, and individual responsibility can make a big difference in preventing and managing these conditions.
✅ Takeaway: Chronic diseases are a silent epidemic, but through awareness, prevention, and healthy lifestyle choices, we can reduce their impact and live healthier lives.
High Cortisol Levels: Symptoms, Causes, and When to Seek Help by nutritionist Laiba Imran
High Cortisol Levels: Symptoms, Causes, and When to Seek Help
As a nutritionist, I often see clients experiencing health issues linked to stress and hormone imbalances. One of the most important hormones in this conversation is cortisol. While it’s normal for cortisol levels to rise and fall throughout the day, consistently high cortisol can harm your health. Doctors call this Cushing’s syndrome or hypercortisolism.
Let’s look at the symptoms, causes, and when to see a doctor, along with some nutrition insights.
Symptoms of High Cortisol
High cortisol can show up in different ways, and the intensity often depends on how long your levels have been elevated. Here’s what to look out for:
-
Weight gain – Often noticeable in the face (creating a “moon face” look), upper back (between the shoulder blades), and abdomen. Unlike typical weight gain, this happens relatively quickly, even without major dietary changes.
-
Acne and skin issues – Breakouts are usually inflammatory and can appear on the face, chest, or back. Skin may also feel oilier than usual. At the same time, skin becomes thinner and heals slowly, leading to easy bruising.
-
Facial flushing – A reddish, flushed appearance across the cheeks.
-
Muscle weakness – Especially in the upper arms and thighs, making everyday tasks (climbing stairs, lifting groceries) more difficult.
-
Severe fatigue – Feeling drained despite adequate sleep, often paired with brain fog and difficulty concentrating.
-
Mood changes – Irritability, restlessness, or even anxiety and low mood.
-
Headaches – Linked to elevated blood pressure and tension from chronic stress.
-
Other changes – High blood pressure, poor wound healing, and in some women, unwanted facial or body hair (hirsutism).
Causes of High Cortisol
Your adrenal glands release cortisol under the direction of your brain (hypothalamus and pituitary gland). When this system is overstimulated, cortisol production can go into overdrive. Common causes include:
Chronic Stress
The body’s “fight-or-flight” response raises cortisol. In modern life, stress may come from work, finances, relationships, or lack of sleep.
Unlike short bursts of stress, chronic stress keeps cortisol high, affecting metabolism, weight, and immunity.
Pituitary Gland Problems
Tumors (usually benign) in the pituitary gland can lead to excess ACTH production, signaling the adrenal glands to release too much cortisol.
Adrenal Gland Tumors
Tumors (benign or malignant) in the adrenal glands may secrete excess cortisol directly. These can sometimes cause abdominal discomfort if large.
Medication Side Effects
Long-term use of corticosteroids (like prednisone, hydrocortisone, or dexamethasone) can mimic the effects of high cortisol.
Stopping corticosteroids suddenly is dangerous—always taper under medical guidance.
When to Contact a Doctor
If you notice several of these symptoms—particularly rapid weight gain in the face or belly, stubborn acne, muscle weakness, or extreme fatigue—it’s important to consult a doctor.
Doctors may recommend:
-
Blood, saliva, or urine cortisol tests to measure hormone levels.
-
Imaging (MRI or CT scans) to look at the pituitary or adrenal glands.
High cortisol increases your risk of heart disease, osteoporosis, and diabetes, so early detection is key.
Nutritionist’s Perspective: Supporting Cortisol Balance
While medical treatment is essential for Cushing’s syndrome, nutrition and lifestyle also play a role in managing stress-related cortisol elevations.
-
Stabilize blood sugar → Eat balanced meals with lean proteins, healthy fats, and complex carbs (e.g., salmon with quinoa and vegetables). Skipping meals or eating sugary snacks causes blood sugar crashes that trigger cortisol release.
-
Support skin health → Vitamin C (citrus fruits, kiwi, bell peppers) supports collagen, helping with skin healing and acne. Zinc-rich foods (pumpkin seeds, chickpeas) aid skin repair.
-
Anti-inflammatory foods → Omega-3s (walnuts, flaxseeds, fish) can reduce inflammation linked to cortisol.
-
Limit stimulants → Too much caffeine or processed sugar worsens cortisol imbalance.
-
Hydrate → Dehydration itself is a mild stressor that raises cortisol.
Takeaway
High cortisol is more than just “stress.” It can cause noticeable weight gain, stubborn acne, fatigue, and muscle weakness. Causes range from stress to medical conditions like pituitary or adrenal tumors.
If you suspect high cortisol, see a doctor for proper testing. Alongside medical care, a balanced diet, regular movement, good sleep, and stress management strategies are powerful tools for supporting hormone balance.
What is Cortisol? by nutritionist by Laiba Imran
What is Cortisol?
Cortisol is a steroid hormone made by your adrenal glands. It’s sometimes called the “stress hormone” because your body releases more of it during stress. But cortisol does much more than that—it supports almost every organ and system in your body.
Its main functions include:
-
Regulating how your body uses glucose (sugar) for energy.
-
Helping manage inflammation.
-
Supporting normal blood pressure.
-
Playing a role in your sleep–wake cycle.
Maintaining the right balance of cortisol is essential—both high and low levels can affect your health.
Cortisol and Stress
Yes, cortisol is strongly linked to stress. When you experience stress (whether short-term, chronic, or traumatic), your body releases cortisol to keep you alert and supply energy by raising blood sugar. But while occasional rises are normal, long-term high levels can be harmful.
How Cortisol Affects Your Body
-
Stress Response: Works with adrenaline to keep you on high alert.
-
Metabolism & Blood Sugar: Balances insulin and glucagon, influencing fat, liver, and muscle tissue.
-
Inflammation: Reduces inflammation short-term, but long-term high cortisol weakens immunity.
-
Blood Pressure: Helps regulate it, but too much raises BP and too little lowers it.
Sleep–Wake Cycle: Peaks in the morning to help you wake up, lowers at night to prepare for rest. Causes and Symptoms of Imbalance
-
High Cortisol (Cushing’s Syndrome): Weight gain (especially around the belly and face), muscle weakness, diabetes, high BP, purple stretch marks, osteoporosis.
-
Low Cortisol (Adrenal Insufficiency): Fatigue, weight loss, low appetite, low BP.
Nutritionist’s Advice: Diet to Support Healthy Cortisol Levels
While medical treatment is required for serious cortisol disorders, your daily food choices can help support balance.
Foods that may help regulate cortisol:
-
Complex carbs (whole grains, oats, quinoa, brown rice): Support steady blood sugar, preventing cortisol spikes.
-
Lean protein (fish, chicken, eggs, legumes): Helps maintain muscle and stabilizes energy.
-
Vitamin C-rich foods (oranges, strawberries, bell peppers): Shown to help lower cortisol after stress.
-
Magnesium-rich foods (leafy greens, nuts, seeds, avocados): Support relaxation and reduce stress responses.
-
Omega-3 fatty acids (salmon, chia seeds, walnuts): May help lower inflammation and stress hormones.
-
Herbal teas (chamomile, green tea in moderation): Can promote calmness and better sleep.
Foods and habits that may raise cortisol if consumed too much:
-
Excess caffeine (coffee, energy drinks).
-
Refined sugars and processed snacks.
-
High intake of alcohol.
-
Skipping meals (causes blood sugar crashes, triggering cortisol release).
Lifestyle + Nutrition Tips to Lower Cortisol Naturally
-
Get quality sleep: Aim for 7–9 hours.
-
Stay active: Regular exercise helps regulate hormones.
-
Eat balanced meals: Avoid long gaps between meals to keep blood sugar stable.
-
Practice stress management: Breathing exercises, meditation, or even laughter help reduce cortisol.
-
Build strong connections: Supportive relationships buffer stress.
What Is a Hormonal Imbalance? by nutritionist Laiba Imran
What Are Hormones?
Hormones are chemical messengers that travel through your bloodstream and tell your organs, skin, muscles, and other tissues what to do and when to do it. They’re absolutely essential for your health and survival.
So far, scientists have identified more than 50 different hormones in the human body. Together with the glands and tissues that produce and release them, hormones make up your endocrine system. This system plays a huge role in keeping your body balanced and functioning properly. Hormones regulate:
- Metabolism (how your body turns food into energy)
- Homeostasis (your body’s internal balance)
- Growth and development
- Sexual function and reproduction
- Sleep and wake cycles
- Mood and emotional health
What Is a Hormonal Imbalance?
A hormonal imbalance happens when your body has either too much or too little of one or more hormones. Because hormones are so powerful, even a slight shift can affect your body in big ways.
Some imbalances are temporary and may fix themselves. Others can be long-term (chronic) and may need treatment to protect your health or quality of life.
Conditions Linked to Hormonal Imbalances
There are many health conditions tied to hormone issues. Here are some of the most common:
- Irregular menstruation (periods): Hormonal conditions like polycystic ovary syndrome (PCOS) or amenorrhea (missed periods) can disrupt the menstrual cycle.
- Infertility: Imbalances are a leading cause of infertility in women (such as with PCOS or anovulation), and men can also experience fertility issues due to low testosterone (hypogonadism).
- Acne: Hormones—especially during puberty—can trigger oil glands and lead to clogged pores.
- Hormonal acne (adult acne): Often linked to pregnancy, menopause, or testosterone therapy, when hormonal changes increase skin oil production.
- Diabetes: The most common hormone-related condition in the U.S. It happens when the pancreas doesn’t make enough insulin or the body can’t use it properly. This includes Type 1, Type 2, and gestational diabetes.
- Thyroid disease: Both hypothyroidism (too little thyroid hormone) and hyperthyroidism (too much) affect metabolism and overall health.
- Obesity: Hormones like cortisol and thyroid hormones influence how your body stores fat and signals hunger. Imbalances can contribute to weight gain.
Symptoms of Hormonal Imbalances
Because you have more than 50 hormones, symptoms vary widely depending on which ones are off balance. These symptoms can overlap with other health conditions, so it’s always important to check with your healthcare provider if you notice changes.
- Metabolism-related symptoms:
- Slow or rapid heartbeat
- Unexplained weight gain or weight loss
- Fatigue
- Constipation or diarrhea
- Numbness or tingling in your hands
- High cholesterol levels
- Depression or anxiety
- Sensitivity to heat or cold
- Dry, coarse skin and hair or thin, moist skin
- Irregular fat distribution
- Dark patches of skin (acanthosis nigricans)
- Skin tags
- Extreme thirst and frequent urination
- Female sex hormone imbalance symptoms:
- Acne (face, chest, back)
- Hair loss
- Heavy or irregular periods
- Excess body hair (hirsutism)
- Hot flashes
- Infertility
- Vaginal dryness or atrophy
- Low sex drive
- Male sex hormone imbalance symptoms:
- Hair loss or reduced body hair
- Erectile dysfunction (ED)
- Enlarged breast tissue (gynecomastia)
- Infertility
- Low sex drive
- Loss of muscle mass
Can Hormone Imbalances Affect Weight?
Yes. Certain hormonal conditions can directly contribute to weight gain:
- Hypothyroidism: Low thyroid hormone slows metabolism, often leading to weight gain.
- Cushing’s syndrome: Too much cortisol can cause fat to build up in the face (“moon face”), neck (“buffalo hump”), belly, and chest.
- Menopause: Metabolism naturally slows, making weight gain common.
Of course, lifestyle factors and other health issues can also play a role.
Can Hormone Imbalances Cause Anxiety?
Absolutely. Hormones don’t just affect your body; they influence your mood and mental health, too.
- Hyperthyroidism: Too much thyroid hormone speeds up your metabolism and can cause anxiety, nervousness, and irritability.
- Cushing’s syndrome: Excess cortisol sometimes leads to anxiety, depression, or irritability.
- Adult-onset growth hormone deficiency: Linked to higher rates of anxiety and depression.
What Causes Hormonal Imbalances?
Your hormone levels naturally rise and fall throughout life—and even throughout the day. Big hormonal shifts are normal during:
- Puberty
- Pregnancy
- Menopause
But outside of these times, several factors can trigger imbalances:
- Stress
- Certain medications
- Steroid use
These are often temporary. But some conditions can cause long-term imbalances, including:
- Tumors or growths (like adenomas or thyroid nodules) that disrupt hormone production
- Damage or injury to endocrine glands (from surgery, infections, radiation, or trauma)
- Autoimmune diseases like Hashimoto’s, Graves’ disease, Type 1 diabetes, and Addison’s disease
Diagnosing Hormonal Imbalances
Doctors usually start with blood tests to measure hormone levels. Since hormones can fluctuate during the day, additional tests (like glucose or insulin tolerance tests) may be needed.
Your medical history, symptoms, and a physical exam all help guide the diagnosis.
Treatment Options
Treatment depends on whether hormone levels are too high or too low:
Low hormone levels: Replaced with hormone therapy (like thyroid pills for hypothyroidism or injections for growth hormone deficiency).
High hormone levels: Options include medication, surgery, radiation, or a combination. For example, a prolactinoma (benign tumor causing excess prolactin) may be treated with medication or removed surgically.
Can You Fix Hormonal Imbalance Naturally?
Some conditions—like diabetes or thyroid disease—require medical treatment. But alongside medical care, lifestyle changes can make a huge difference in supporting hormone health:
- Eating a balanced, nutrient-dense diet
- Managing stress effectively
- Exercising regularly
- Getting enough quality sleep
- Avoiding smoking and tobacco
- Maintaining a healthy weight
- Staying on top of chronic health conditions
Who Treats Hormonal Imbalances?
Your primary care doctor can diagnose and manage many imbalances. But for complex cases, you may need an endocrinologist, a specialist in hormone health. They can develop personalized treatment plans and prescribe the right medication if needed.
Can Hormonal Imbalances Be Prevented?
Not all of them—but you can lower your risk and keep your hormones as balanced as possible by focusing on overall wellness:
- Eat a nourishing, balanced diet
- Stay physically active
- Manage your stress levels
- Prioritize good sleep
- Keep a healthy weight
- Quit smoking, if you smoke
HPV VACIINE UPDATES REPORT BY HANZAL
“The HPV vaccine is safe, free, and available to every eligible girl. By protecting their health today, we are safeguarding their education, their future, and their ability to contribute to society. Let us keep this momentum going until every eligible girl is reached,” Dr Bharath said.
Hormones and Their Role in Health by nutritionist Laiba Imran
Hormones and Their Role in Health
Hormones are chemical messengers that play a vital role in coordinating and regulating different functions in your body. They travel through your bloodstream to organs, muscles, skin, and other tissues, sending signals that tell the body what to do and when to do it. In this way, hormones influence everything from your metabolism and growth to your mood and reproductive health.
So far, scientists have identified over 50 different hormones in the human body. Most of these hormones are produced and released by glands in your endocrine system, but other tissues—such as fat, kidneys, liver, and even your digestive tract—also produce hormones or hormone-like substances.
Because hormones are powerful, even a small change in their levels can significantly affect health. Minor imbalances can lead to symptoms, while larger ones can cause medical conditions that may require treatment.
What Hormones Do
Hormones affect and manage hundreds of bodily processes, often working in chain reactions with other hormones. They regulate:
Metabolism (turning food into energy).
Homeostasis, or internal balance (blood sugar, blood pressure, fluid and electrolyte balance, and body temperature).
Growth and development.
Sexual function and reproduction.
Sleep-wake cycle.
Mood and behavior.
Hormones work like keys that fit into specific locks—the receptors on target cells. If the hormone “fits,” it delivers its message and triggers the cell or organ to take action.
There are two main types of hormone communication:
Between two endocrine glands — for example, the pituitary gland releases thyroid-stimulating hormone (TSH), which signals the thyroid gland to release its hormones that affect metabolism.
Between a gland and a target organ — for example, the pancreas releases insulin, which acts on the liver and muscles to help regulate glucose.
Which Tissues Make Hormones?
The endocrine system is the main network of glands that produce hormones. It includes:
Hypothalamus: Controls the pituitary gland and makes hormones like corticotrophin-releasing hormone, dopamine, growth hormone-releasing hormone, and thyrotropin-releasing hormone. It also produces oxytocin (stored and released by the pituitary) and somatostatin.
Pituitary gland: Known as the “master gland,” it produces hormones that control other glands. The anterior pituitary makes ACTH, FSH, GH, LH, prolactin, and TSH. The posterior pituitary releases antidiuretic hormone (ADH/vasopressin) and oxytocin.
Pineal gland: Produces melatonin, which regulates sleep-wake cycles.
Thyroid gland: Produces thyroxine (T4), triiodothyronine (T3), reverse T3, and calcitonin, all of which regulate metabolism and calcium balance.
Parathyroid glands: Release parathyroid hormone (PTH), which maintains calcium balance and bone health.
Adrenal glands: Located on top of the kidneys, they produce cortisol, aldosterone, DHEA and androgens, adrenaline (epinephrine), and noradrenaline (norepinephrine).
Pancreas: Produces insulin and glucagon, both essential for blood sugar regulation.
Ovaries (in women): Produce estrogen, progesterone, and small amounts of testosterone.
Testes (in men): Produce sperm and testosterone.
Other hormone-producing tissues include:
Adipose tissue (fat): Produces leptin, adiponectin, plasminogen activator inhibitor-1, estrogen, and angiotensin.
Kidneys: Release erythropoietin, renin, and the active form of vitamin D (actually a prohormone).
Liver: Produces insulin-like growth factor 1 (IGF-1) and angiotensinogen.
Gut (gastrointestinal tract): Produces ghrelin, somatostatin, and GLP-1, which influence appetite and digestion.
Placenta (during pregnancy): Produces estrogen and progesterone to support fetal development and maintain pregnancy.
Conditions Caused by Hormone Issues
Too much or too little of a hormone can disrupt balance and lead to health problems. Common hormone-related conditions include:
Diabetes (Type 1, Type 2, and gestational diabetes).
Thyroid disorders (hypothyroidism and hyperthyroidism).
Polycystic ovary syndrome (PCOS), irregular periods, and infertility in women.
Low testosterone (hypogonadism) and infertility in men.
Obesity, often linked with imbalances in leptin, insulin, or cortisol.
Causes of Hormonal Imbalances
Hormone imbalances can result from:
Tumors or adenomas (growths on glands).
Injury or damage to an endocrine gland.
Autoimmune diseases (e.g., Type 1 diabetes).
Genetic mutations that affect hormone production or gland function.
Who Treats Hormonal Conditions?
Many hormone conditions can be managed by a primary care doctor, but more complex cases are treated by an endocrinologist—a specialist in hormone health. Endocrinologists diagnose, manage, and treat disorders related to the endocrine system, often with medications or hormone replacement therapies.
Hormones and Women’s Health
Hormones are critical for both men and women, but women tend to experience more frequent and intense hormonal changes due to major life stages such as puberty, pregnancy, and menopause.
While men also have estrogen, progesterone, and other hormones, they don’t experience the same sudden shifts and fluctuations that women do. These hormonal changes in women often lead to noticeable symptoms—ranging from mood swings and sleep changes to fertility challenges—that can affect daily life and long-term health.