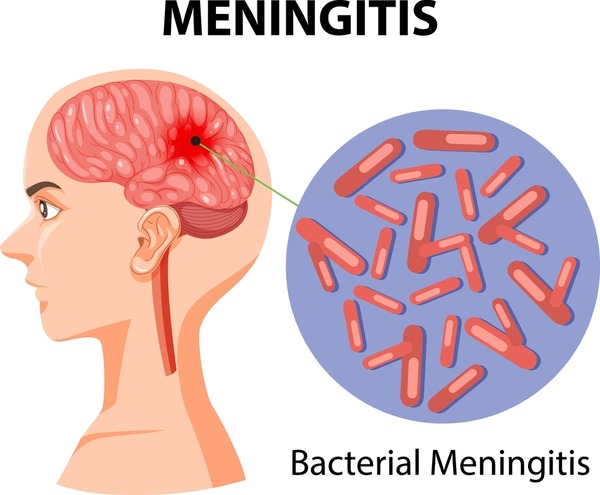
- Bacterial meningitis is a serious infection of the protective membranes (meninges) surrounding the brain and spinal cord. While it is not very common, it can progress rapidly and become life-threatening if not treated quickly. Understanding the condition, its warning signs, and ways to prevent it can save lives.
What is Bacterial Meningitis?
Meningitis refers to the inflammation of the meninges. When caused by bacteria, it is called bacterial meningitis. The infection leads to swelling, which can disrupt the normal function of the brain and spinal cord.
Unlike viral meningitis, which is often mild, bacterial meningitis requires immediate medical care.
Common Bacteria That Cause Meningitis Several bacteria can trigger this illness:
- Neisseria meningitidis (meningococcus) – often causes outbreaks.
- Streptococcus pneumoniae (pneumococcus) – the most common cause in infants and adults.
- Haemophilus influenzae type b (Hib) – used to be common, now rare due to vaccines.
- Group B Streptococcus – often affects newborns.
- Listeria monocytogenes – more common in pregnant women, newborns, and older adults.
Symptoms to Watch Out For:
Symptoms can appear suddenly within hours or develop over a few days. Key warning signs include:
- Severe headache
- Stiff neck
- Fever and chills
- Sensitivity to light (photophobia)
- Nausea and vomiting
- Confusion or difficulty concentrating
- Seizures
- In infants: bulging soft spot, poor feeding, irritability
How is it Diagnosed?
Doctors usually confirm bacterial meningitis through:
- Lumbar puncture (spinal tap): checks cerebrospinal fluid (CSF) for bacteria.
- Blood tests: to identify infection.
- Imaging (CT or MRI): sometimes needed to rule out other causes.
Treatment Options
Bacterial meningitis requires urgent hospitalization. Treatment usually includes:
Intravenous (IV) antibiotics – started immediately.
Corticosteroids – to reduce brain inflammation.
Supportive care – for fever, seizures, or dehydration.
Early treatment improves survival and reduces complications such as hearing loss, brain damage, or learning difficulties.
Prevention: Can Meningitis Be Avoided?
Yes – many cases can be prevented through:
1. Vaccination:
- Hib vaccine
- Meningococcal vaccine
- Pneumococcal vaccine
2. Good hygiene: Handwashing, not sharing utensils, covering mouth when coughing.
3. Healthy lifestyle: Strong immunity lowers infection risk.
4. Antibiotic prophylaxis: Close contacts of meningitis patients may be given preventive antibiotics.
Bacterial meningitis is a medical emergency that should never be ignored. While it can strike suddenly, awareness, early diagnosis, and timely treatment can make the difference between life and death. Vaccination remains the strongest shield against this dangerous infection.