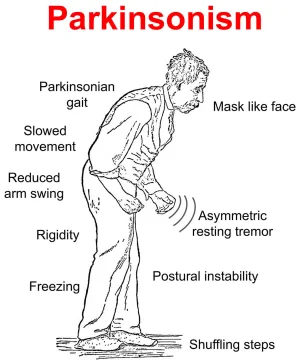
Parkinsonism is a clinical syndrome characterized by a group of movement abnormalities that resemble those seen in Parkinson’s disease (PD) It is not a single disease, but rather a set of signs and symptoms caused by various underlying conditions or factors that affect the dopaminergic system in the brain (especially the basal ganglia).
⚠️ Common Symptoms:
Key symptoms of parkinsonism usually include motor and some non-motor features:
~ Motor symptoms
~ Bradykinesia– slowness of movement (core feature)
~ Rigidity– muscle stiffness
~ Resting tremor – shaking when muscles are at rest
~ Postural instability impaired balance and coordination
~Shuffling gait small steps, stooped posture
~ Non-motor symptoms
~ Cognitive impairment or dementia (in some types)
~ Depression, anxiety, apathy
~ Sleep disturbances
~ Autonomic dysfunction (constipation, orthostatic hypotension, urinary issues)
⚠️ Causes:
Parkinsonism can result from several causes. The main categories include:
1. Neurodegenerative diseases:
Idiopathic Parkinson’s disease (most common cause)
Atypical parkinsonian disorders (e.g., multiple system atrophy, progressive supranuclear palsy, corticobasal degeneration, dementia with Lewy bodies)
2. Secondary parkinsonism:
~ Drug-induced (antipsychotics, antiemetics that block dopamine receptors)
~ Vascular parkinsonism (due to multiple small strokes)
~ Post-traumatic (chronic traumatic encephalopathy)
~ Infections (encephalitis), toxins (manganese, carbon monoxide), metabolic disorders
📊 Prevalence:
Parkinsonism prevalence varies by type.
Idiopathic Parkinson’s disease:
~ Affects about 1% of people over 60 and \~0.3% of the general population worldwide.
~ Risk increases sharply with age.
~ Atypical and secondary parkinsonism:less common, but together may account for 10–20% of all parkinsonism cases seen in clinics.
🥗 Nutritional Intervention:
While no diet can cure parkinsonism, nutritional support can help manage symptoms, improve quality of life, and support medication effectiveness.
General strategies:
Balanced diet: Emphasize fruits, vegetables, whole grains, lean proteins, and healthy fats (Mediterranean-style diet is often recommended).
~Adequate hydration and fiber to relieve constipation (common symptom).
~ Adequate calcium and vitamin D to maintain bone health (due to higher fall risk).
Specific considerations:
~ Levodopa interaction: High-protein meals can interfere with levodopa absorption. Patients may benefit from:
• Spreading protein intake evenly throughout the day
• Taking levodopa 30–60 minutes before meals
~ Antioxidant-rich foods: Berries, leafy greens, nuts (may help combat oxidative stress)
~ Omega-3 fatty acids: Anti-inflammatory effects, potential cognitive benefits
~ Monitor weight: Both unintended weight loss (due to swallowing difficulties or reduced appetite) and weight gain (due to reduced activity) can occur.